Etiology of Acute Kidney Injury (AKI) in Hospitalized Patients - #5
Take QuizReview etiolgies of acute kidney injury in hospitalized patients.
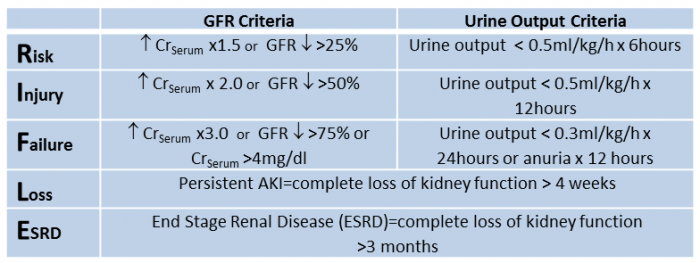
The RIFLE criteria can aid in accurate staging of patients with AKI. This system includes 3 levels of renal dysfunction (R-risk, I-injury, F-failure; have higher sensitivity) and 2 levels of clinical outcomes (L-loss, E-ESRD; have higher specificity).
Etiologies of AKI
Prerenal AKI
Decreased renal perfusion -The elderly may be more susceptible to AKI in a low perfusion state because of attenuated responses to vasodilators and an increase in response to vasoconstrictors. Volume depletion, hypotension, and congestive heart failure (CHF) are causes of perfusion related AKI.
Sepsis - Increasing evidence suggests that sepsis-associated AKI is an inflammatory event. Serum interleukin-6 levels may predict incidence of AKI, as well as severity and mortality among patients admitted to the ICU with acute respiratory distress syndrome or community-acquired pneumonia.
Renal AKI
Acute Tubular Necrosis (ATN) - Most frequent cause of AKI in elderly patients. Insults leading to ATN include nephrotoxins (radiocontrast, aminoglycosides)pigment-induced (rhabdomyolysis can occur after a fall with a long lie),and ischemia (sepsis, surgery).
Renovascular disease - acute obstruction of the renal vasculature (cholesterol emboli following intravascular surgery, renal artery thrombosis)
Normotensive ischemic AKI - Normally, a decrease in mean arterial pressure results in preservation of the GFR at mean arterial pressures between 80-100 mm Hg. In patients with impaired renal autoregulation, the GFR is not preserved at these pressures resulting in normotensive ischemic damage. Autoregulation is impaired by non steroidal anti-inflammatory drugs, angiotensin-converting enzyme inhibitors, and angiotensin receptor antagonists.
Acute Interstitial Nephritis - Common practice of polypharmacy in the elderly puts this population at increased risk of having an adverse event that damages the kidney. This includes herbal supplements and over the counter prescription medications in addition to prescription medications such as antibiotics (i.e. β lactam-containing antibiotics such as methicillin).
Postrenal AKI
Obstruction
- Ureter (Pelvic malignancy, e.g. invasive cervical carcinoma), Bladder (carcinoma)
- Prostate (benign prostatic hyperplasia, carcinoma), Urethra (stricture secondary to trauma, pelvic malignancy)
Tap on Image to Enlarge
Geriatric patient in a hospital or other healthcare facility
Response to an increasing serum creatinine or decreasing urine output in a geriatric inpatient.
Acute kidney injury (AKI), as defined by the precipitous decline in glomerular filtration rate (GFR), is frequently encountered in the elderly patient. The decreased renal reserve and the associated co-morbid conditions of elderly patients (e.g., hypertension, diabetes, heart failure, vascular disease) increase the risk for the development of AKI. AKI in the geriatric population has been estimated to be somewhere between 1.5% and 7.0% using Medicare billing codes over the last 30 years. The RIFLE criteria can aid in accurate staging of patients with AKI.; This system includes 3 levels of renal dysfunction (R-risk, I-injury, F-failure; have higher sensitivity) and 2 levels of clinical outcomes (L-loss, E-ESRD; have higher specificity).
Science Principles
- To recognize common etiologies of AKI in hospitalized geriatric patients
- To review the RIFLE criteria for staging severity of AKI
Review of Systems (ROS)
Geriatric Topics
ACGME Compentencies
Science Principles
- http://www.asn-online.org/education_and_meetings/geriatrics/OnlineGeriat...
- Acute Kidney Injury in the Elderly Clinics in Geriatric Medicine - Volume 25, Issue 3 (August 2009) http://www.ncbi.nlm.nih.gov/pubmed/19765485
- Normotensive Ischemic Acute Renal Failure. J. Gary Abuelo, M.D.N Engl J Med 2007;357:797-805 http://www.ncbi.nlm.nih.gov/pubmed/17715412
Users are free to download and distribute Geriatric Fast Facts for informational, educational, and research purposes only. Citation: Christopher J Anderson, Edmund Duthie, MD, Brahm Vasudev, MD, Bambi Wessel - Fast Fact #005 - Etiology of Acute Kidney Injury (AKI) in Hospitalized Geriatric Patients. February 2012.
Disclaimer: Geriatric Fast Facts are for informational, educational and research purposes only. Geriatric Fast Facts are not, nor are they intended to be, medical advice. Health care providers should exercise their own independent clinical judgment when diagnosing and treating patients. Some Geriatric Fast Facts cite the use of a product in a dosage, for an indication, or in a manner other than that recommended in the product labeling. Accordingly, the official prescribing information should be consulted before any such product is used.
Terms of Use: Geriatric Fast Facts are provided for informational, educational and research purposes only. Use of the material for any other purpose constitutes infringement of the copyright and intellectual property rights owned by the specific authors and/or their affiliated institutions listed on each Fast Fact. By using any of this material, you assume all risks of copyright infringement and related liability. Geriatric Fast Facts may not be reproduced or used for unauthorized purposes without prior written permission, which may be obtained by submitting a written request to: Medical College of Wisconsin, Dept. of Medicine, Division of Geriatrics and Gerontology, 8701 Watertown Plank Road, Milwaukee, WI 53226. Note the Geriatric Fast Facts may contain copyrighted work created under contract with government agencies, foundations, funding organizations and commercial companies, etc. If a particular author places further restrictions on the material, you must honor those restrictions regardless of whether such restrictions are described in this mobile app.